📌 Quick Guide: 4 Key Facts About Tooth Decay
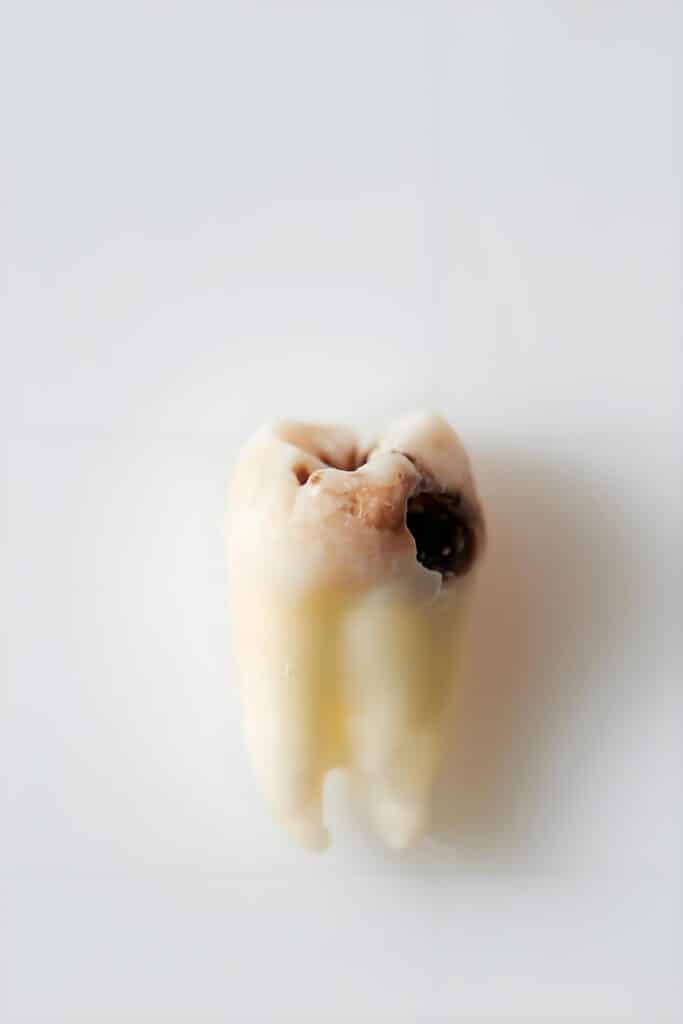
🔍 Symptoms: White spots, black lines, or small holes on the tooth surface; brief sharp pain when exposed to hot, cold, or sweet stimuli; spontaneous pain without any trigger, especially at night.
🦷 Typical Treatment Approach:
- Early decay (no cavity) → Fluoride application
- Decay reaching dentin (small area) → Filling
- Decay reaching dentin (large area) → Crown
- Decay reaching the pulp → Root canal treatment + crown; otherwise, extraction may be needed
💰 Cost Reference:
- Filling: from $900
- Root canal treatment (per tooth): from $6,600
- Crown / Bridge / Inlay / Veneer (per unit): from $7,700
(Based on Prince Philip Dental Hospital fee schedule)
💡 Key Takeaway: Tooth decay is irreversible. The earlier you seek treatment, the more you save on costs and preserve your natural teeth. A check‑up every 6 to 12 months is the best way to prevent decay.
How Does Tooth Decay Form? — The “Quartet” of Cavities
Oral bacteria are the true culprits behind tooth decay. After we eat, food debris—especially sugar—lingers on the tooth surface, and a battle begins inside the mouth:
1️⃣ Bacterial Army Assembles
Streptococcus mutans and Lactobacillus are the main drivers of this destruction. When sugar from food debris enters the mouth, these bacteria produce an enzyme that turns sugar into a sticky, glue‑like substance. This “cement” helps them cling tightly to the tooth surface, forming a biofilm called dental plaque—invisible to the naked eye.
2️⃣ The Acid Attack
Bacteria in plaque use sugar as fuel and launch into a metabolic frenzy. One gram of plaque can harbor 10 billion bacteria, and each milliliter of plaque fluid can contain up to 1,000 mg of lactic acid. When the pH drops below 5.5, the hydroxyapatite in tooth enamel begins to dissolve. This demineralization process is like “ants gnawing at a bone.” Initially, it shows only as chalky white spots, but beneath the surface, tooth structure is quietly being damaged.
3️⃣ Structural Collapse Underway
Ongoing acid erosion creates tiny pores in the enamel, opening pathways for bacteria. When the destruction reaches the dentin, the tubular structure amplifies external stimuli, causing sensitivity to hot and cold. Worse still, Streptococcus mutans can produce extracellular polysaccharides that build an “acid barrier” within the plaque, blocking the calcium and phosphate ions in saliva from carrying out remineralization.
4️⃣ Chain Reaction of Ecological Imbalance
Modern research shows that tooth decay is caused by an imbalance in oral bacteria. In a healthy mouth, good bacteria keep harmful bacteria in check. But a high‑sugar diet disrupts this balance—frequent sugar intake lowers oral pH, creating an acidic environment where decay‑causing bacteria thrive while good bacteria cannot survive. This is dysbiosis: harmful bacteria multiply, healthy bacteria are suppressed, and teeth begin to break down. An increase in certain bacteria in plaque is also linked to root surface cavities, accelerating damage to the tooth root.
Related Reading: Oral microecological community — Streptococcus mutans dysbiosis and interaction provide therapeutic perspectives for dental caries
The Four Stages of Tooth Decay: From No Sensation to Severe Pain
| Stage | Signs & Sensations | What to Do |
| Stage 1: Early Enamel Decay | Chalky white spots or fine black lines appear on the tooth surface. No pain. | Apply fluoride or have a filling as soon as possible. Do not ignore it just because there is no pain—early treatment prevents the decay from getting worse. |
| Stage 2: Cavity Formation | The enamel is damaged and a visible cavity forms. The tooth becomes sensitive to hot, cold, or sweet foods and drinks. | A filling is usually sufficient. The longer you wait, the larger the cavity becomes and the more complex the treatment will be. |
| Stage 3: Pulpitis (Pulp Inflammation) | Spontaneous pain, pain that worsens at night, pain that radiates to other areas, and prolonged pain after hot or cold stimulation. | Root Canal Treatment (RCT) is needed. If you experience these symptoms, seek dental care promptly. |
| Stage 4: Pulp Necrosis | Pain temporarily subsides, but bacteria spread to the tooth root, possibly forming an abscess. | Root Canal Treatment (RCT) or Tooth Extraction. If the root infection is severe, the tooth may not be able to be saved. |
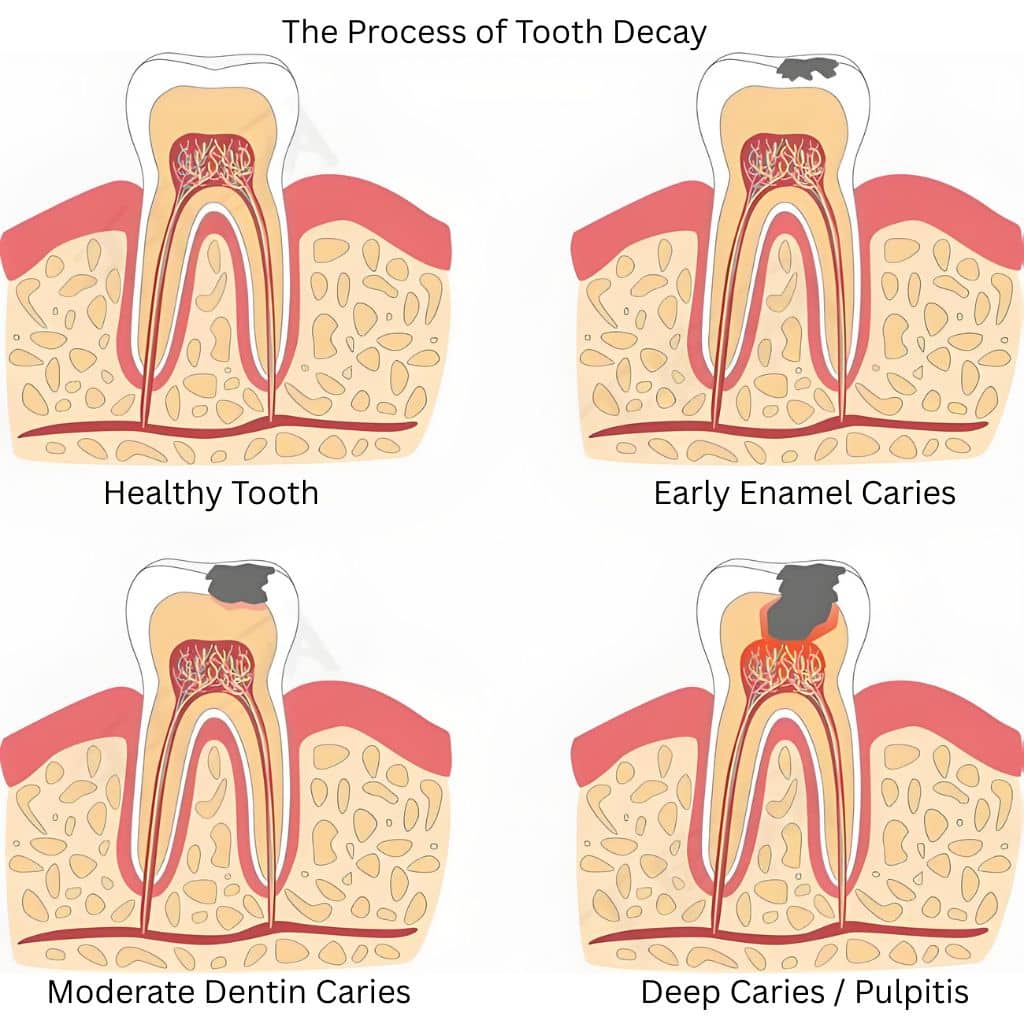
Stages of Tooth Decay Progression
💡 Our Root Canal Treatment (RCT) Approach
We provide professional Root Canal Treatment (RCT) focused on preserving your natural tooth:
- Accurate Diagnosis: Using X-rays and digital scans, we precisely assess the extent of pulp infection and develop a personalized treatment plan tailored to your needs.
- Microscope‑Assisted Treatment: A surgical microscope is used throughout the procedure, clearly displaying the process on a screen. This allows for precise removal of infected pulp tissue, improving treatment success.
- Biocompatible Filling: After cleaning, the canals are filled with a high‑quality biocompatible material to prevent reinfection and seal the tooth.
- Crown Protection: A dental crown is recommended after treatment to protect the weakened tooth structure and extend its longevity.
The entire treatment typically requires 2 to 3 visits, each lasting about 60 to 90 minutes. Local anaesthesia is used to ensure a comfortable, pain‑free experience. Some mild swelling or discomfort may occur after treatment—this is normal and can be managed with pain relief as advised.
Bayside Dental Tung Chung | Same‑Day Appointments Available
2026 Cavity Treatment Options & Cost Reference
The following prices are based on the Private Patient Fee Schedule of The Prince Philip Dental Hospital and are for reference only. Actual fees charged by private dental clinics may vary depending on the dentist’s experience, equipment used, clinic location, and case complexity. Please consult your dentist for an accurate quote.
| Treatment Item | Fee Range (HKD) | Indications |
| Restoration | $900 – $3,000 | Small cavity; tooth structure remains strong |
| Root Canal Therapy (per tooth) | $6,600 – $25,000 | Decay has spread to the dental pulp |
| Crown/Bridge/Onlay/Inlay/Veneer (per unit) | $7,700 – $12,000 | Extensive decay; tooth structure is weakened |
| Simple Extraction | $700 – $2,000 | When root canal treatment is not possible |
| Removal of Wisdom Tooth | $5,000 – $10,000 | Impacted or complex cases |
💡 Note: The above prices are for reference only. Actual costs depend on the dental clinic’s equipment, the dentist’s experience, and the complexity of the case. In addition to the fees listed, charges may apply for dental appliances, precious alloys, mini bone plates, mini screws, posts, and other cost‑recoverable items.
5 Steps to Prevent Tooth Decay
- Correct Brushing Technique: Brush your teeth twice a day, for at least two minutes each time, using fluoride toothpaste. It is recommended to use the 45° Bass brushing technique (place the toothbrush at a 45‑degree angle to the gum line and use gentle vibrating movements), or vertical brushing and small circular motions to ensure all tooth surfaces are cleaned.
- Use Dental Floss or Interdental Brushes: Clean between your teeth at least once a day—this is key to preventing cavities on the adjacent surfaces.
- Watch Your Diet: Reduce intake of high‑sugar foods and drinks (such as candy, cake, and soda). Rinse your mouth with water after eating.
- Regular Check‑ups: The Hong Kong Department of Health recommends that everyone have a dental check‑up at least once a year. Children, those who have had cavities before, and people at high risk (e.g., those with a history of tooth decay, periodontal disease, or dry mouth) should consider having check‑ups every 3 to 4 months.
- Pit and Fissure Sealants: For children, pit and fissure sealants can be applied to newly erupted permanent molars to effectively prevent cavities on the chewing surfaces of the back teeth.
Conclusion
What begins as a tiny black line can develop into excruciating pulpitis over the course of months to years. Early treatment may require only a simple filling costing a few hundred dollars. Once the pulp becomes inflamed, however, the cost of root canal treatment multiplies, and the tooth itself loses vitality, becoming weak and prone to fracture.
Key points:
✅ Have a dental check‑up at least once a year to detect chalky white spots, black lines, and cavities early.
✅ If you experience spontaneous pain, night pain, radiating pain, or prolonged discomfort after hot or cold stimulation, these are signs of pulp inflammation—seek dental care promptly.
Frequently Asked Questions About Cavities
Can early‑stage tooth decay that causes no pain be ignored?
No. Early‑stage decay affects only the enamel. Although there is no pain at this stage, bacteria are still actively damaging the tooth structure. Timely fluoride application or a filling can prevent the cavity from reaching the dentin or pulp, avoiding more complex and costly treatment later.
What materials are used for fillings? What are the differences?
The choice of filling material depends on the location, size of the cavity, and aesthetic needs. Common options include:
• Composite Resin: Matches natural tooth colour, highly aesthetic. Ideal for front teeth and small cavities. This is the most commonly used material.
• Amalgam (Silver Filling): Highly durable and more affordable. Suitable for back teeth, but its noticeable colour makes it less common for front teeth.
• Ceramic: Close to natural tooth colour, stain‑resistant, and ideal for areas where aesthetics are important, but it is more expensive.
• Gold Alloy: Extremely strong, corrosion‑resistant, and long‑lasting. Suitable for back teeth, though it is the most expensive option and its colour is noticeable.
Your dentist will recommend the most suitable material based on the cavity’s location, the extent of damage, aesthetic needs, and your budget.
Will I feel pain after a filling? How long until I can eat normally?
You may experience temporary sensitivity to hot or cold after a filling, which usually subsides within a few days. If the cavity was deep, your dentist may advise avoiding chewing hard food with that tooth for about 24 hours to allow the filling material to fully set. After that, you can resume a normal diet. If pain persists or you feel discomfort when biting, you should schedule a follow‑up visit.
Why can a tooth get decayed again after being filled?
Recurrent decay can occur for several reasons: poor oral hygiene, tiny gaps that form between the filling and the tooth, or the decay extending beyond the original area of the filling. Maintaining good brushing habits, flossing daily, and attending regular check‑ups are essential to prevent this.
Can regular dental cleanings (scaling) prevent tooth decay?
Yes. Professional scaling removes calculus (tartar) and stubborn plaque that daily brushing cannot, reducing the number of decay‑causing bacteria. During the cleaning, your dentist can also examine your teeth and detect early signs of decay for prompt treatment. The Hong Kong Dental Association recommends professional cleaning every 6 to 12 months.
Who is at high risk for tooth decay?
• Children and adolescents (teeth are still developing, oral hygiene habits are not yet fully established)
• Individuals who have had cavities before (higher risk of recurrence)
• People with dry mouth (reduced saliva flow lowers the mouth’s natural self‑cleaning ability)
• Those wearing braces (food particles and plaque easily accumulate around brackets and wires)
• People with diabetes or those who smoke
Individuals who frequently consume sugary foods or drinks
Do baby teeth with cavities need treatment?
Yes, absolutely. Untreated cavities in baby teeth can affect the development of permanent teeth, lead to unbalanced chewing habits that may cause facial asymmetry, and even impact a child’s nutrition and self‑confidence. Timely filling of decayed baby teeth is a crucial investment in a child’s long‑term health.
What should I do if my wisdom tooth is decayed?
Wisdom teeth are located at the very back of the mouth, making them hard to clean and prone to decay. If the tooth is properly positioned and has an opposing tooth, a filling may be an option. However, if the tooth is misaligned or causes repeated inflammation, your dentist will usually recommend removal to prevent problems with the adjacent teeth.
Why is a dental crown necessary after root canal treatment?
After root canal treatment, the tooth loses its nutrient supply and the existing cavity has already weakened its structure, making it fragile and more likely to crack under biting force. Placing a crown provides 360‑degree protection, significantly extending the tooth’s lifespan.